
Juice WRLD’s death in December 2019 shook a generation. He was 21 years old. The official cause was accidental oxycodone and codeine toxicity.
His passing wasn’t just about opioids. It highlighted something even more dangerous: high tolerance, secrecy, and sudden physiological collapse.
This is the modern opioid pattern.
The Tragic Hook: “He was still performing.”
Juice WRLD had openly discussed substance use in interviews and lyrics. Fans knew the struggle was real.
What many didn’t understand was how fast opioid toxicity can escalate when:
- Tolerance is high
- Dosage is inconsistent
- Stress spikes
- Seizure risk is present
He suffered a medical emergency shortly after landing at Chicago Midway Airport.
The body can only compensate for so long.

Substance Involved (High-Level Summary)
The official toxicology report identified:
- Oxycodone
- Codeine
Both are opioids. Both depress the central nervous system. Together, they increase respiratory suppression risk.
Toxicology Details (Lay Explanation)
Opioids affect the brainstem — the part that controls breathing.
Here’s what happens:
- Breathing slows
- Carbon dioxide rises
- Oxygen drops
- The brain begins to shut down
In some cases, opioid toxicity can also trigger seizures, especially with high-dose ingestion.
Seizures complicate oxygen supply even further.
This is how overdose can turn catastrophic quickly.
The Codeine Culture Risk
Codeine — often consumed as “lean” or cough syrup mixtures — became normalized in parts of music culture.
But codeine is still an opioid.
And when combined with:
- Oxycodone
- Alcohol
- Benzodiazepines
- High doses
- Reduced tolerance after breaks
The margin of safety collapses.
Timeline Pattern in Young Opioid Relapse
The modern relapse sequence often looks like:
- Public success
- Private stress
- Opioid normalization
- High tolerance
- Sudden ingestion spike
- Respiratory depression or seizure
Young users often underestimate the lethality because they feel physically resilient.
Opioids do not care about age.

Warning Signs of Opioid Escalation
If you see these patterns, act early:
- Nodding off unexpectedly
- Pinpoint pupils
- Slurred speech
- Constipation and fatigue
- Mixing cough syrup with alcohol
- Seizure-like activity
- Concealing pill bottles
- Increased isolation
One critical red flag:
Using opioids in high-stress situations while attempting to appear functional.
The Relapse Psychology Section (Short and Direct)
Relapse often starts with confidence:
“I’ve handled more before.”
“I know my limits.”
“I can function.”
Tolerance tricks the brain into believing safety exists.
But tolerance only means the body has adapted — not that it is protected.
When dosage exceeds respiratory capacity, collapse follows.
Seizures and Opioid Toxicity
While respiratory depression is the primary mechanism, seizures can occur in severe intoxication cases.
Seizures:
- Increase oxygen demand
- Disrupt breathing
- Increase cardiac strain
Combined with opioid suppression, outcomes worsen rapidly.

What To Do If You’re Concerned
If someone is:
- Not breathing normally
- Unresponsive
- Turning blue
- Seizing
Call emergency services immediately.
If you’re worried but it’s not yet an emergency:
- Ask directly about opioid use
- Remove access to pills
- Encourage medical evaluation
- Seek addiction assessment
- Consider medication-assisted treatment (MAT)
The earlier intervention begins, the greater the survival odds.
Private Treatment Saves Lives — Act Before It’s Too Late
Juice WRLD’s story reflects a pattern repeating across the country.
Young. Talented. Functional.
Still vulnerable.
Opioid tolerance is not protection.
If someone you love is using opioids or codeine mixtures, waiting is not neutral.
Delay death. Choose treatment.
The Next Step Before It’s Too Late
- Confidential consultation
- Rapid assessment
- MAT options available
- Insurance-friendly placement
- Discreet support
Call now. Don’t wait.
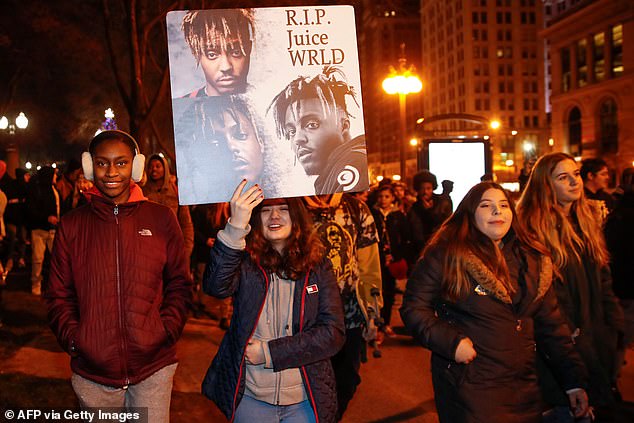

📞 💬The Next Step Before It’s Too Late?
If you or someone you love is struggling with addiction, answer these 3 quick questions to speak with a recovery advisor:
- Do you need inpatient treatment for alcohol or drug addiction?
- Do you have private PPO insurance or $15,000+ available for care?
- Are you willing to travel out of state for treatment? (A change of scenery produces better outcome)
✅ If you answered YES to all 3, tap here to speak with an advisor now. 🔒 100% Confidential.
 Skip to content
Skip to content